The medication and treatments necessary to a vitiligo patient are long term and costly. Depending on the insurance company you are with, they may cover the price of medication, home treatment unit, doctor appointment fees, UV sessions in the doctor’s office or none of the above. The most helpful type of reimbursement is the reimbursement for the UV unit - a hand-held UVB unit may suffice for a patient with few affected areas but if your spots are widespread a panel type unit is necessary, with prices starting around 1000$. Sometimes the insurance company covers part of the price of a UV unit or requires a letter of medical necessity from your doctor to back up your claim. You can suggest your doctor to mention some of the below points in the letter in order to improve the chance of success of your claim: • Emphasize on the benefit for the insurance company on the long run – compare the price for the estimated number of treatments in the doctor’s office costing X $ versus a one time payment for the home unit – costing less; • Mention that other therapies have been applied but with little result. For example mention that the patient is non responsive to topical therapy • Necessity of the device in order to regain pigment and keep the disease from spreading and to avoid severe sunburn – a known cause of skin cancer
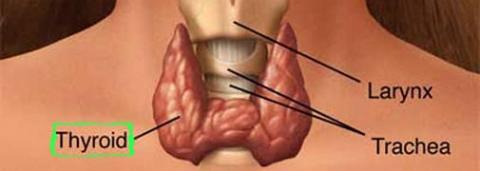
The guidelines for vitiligo treatment published by the British Association of dermatologists in 2008 recommend screening for thyroid disease in vitiligo patients. Findings from a retrospective study performed on Canadian patients support thyroid testing. The study included 300 patients and revealed that 4% of patients who had no thyroid disease reported at admission proved to have increased levels of TSH (thyroid stimulating hormone) - a likely sign of undiagnosed thyroid disease. Taking into account borderline patients (who's TSH values are slightly higher than average, but still in the normal range) the percent of vitiligo patients with thyroid problems rises to 16%. Another study pointed out that an elevated risk of thyroid disease is found among older women and women with a family history of thyroid disease. It appears that thyroid alterations predominantly affect patients with non-segmental vitiligo. In children it was found that 13 out of 121 (10,7%) patients enrolled in a study had different degrees of thyroid parameter alterations. The most common disorders affecting the thyroid are hyperthyroidism and hypothyroidism (an under-active thyroid) and hypothyroidism (an overactive thyroid). A study conducted on 30 patients with vitiligo found hyperthyroidism and hypothyroidism in 10 and 6.6%, respectively.
Due to it's antioxidant function, Ginko Biloba's efficiency in controlling the activity and spread of vitiligo as well as it's usefulness in inducing repigmentation was put to the test by a team of researchers from India. A study published in BMC dermatology shows that 80 percent of the patients treated with 40mg Ginko Biloba three times per day for six months experienced a cessation in the disease progression; 40 percent experienced some degree of repigmentation as compared to only 8 percent in the placebo group.
I once met someone who would not answer at all when asked about his vitiligo spots. I think he never had the time to absorb the changes he was going through and therefore was totally blocking this subject. A person diagnosed with vitiligo might experience anything from loss of self confidence to deep depression. The fear of patches expanding quickly over visible areas can have a high impact around the age when one is most conscious about his appearance. Friends and family can help a person diagnosed with vitiligo in emotionally dealing with the disease. Below are some ideas that may help:
Focal vitiligo is characterized by a few scattered macules. In some cases the depigmenation remains localized to these spots. For others, focal vitiligo can be a manifestation for general vitiligo. Unilateral (segmental vitiligo) In this case the patterns of depigmentatiaon involve small to large areas on one side of one's body. The patterns of depigmentation repeat from patient to patient. The prognostic is different from generalized vitiligo: the disease spreads for 1-2 year in the involved patch,and then the disease stops. There are rare cases where this type of vitiligo progresses to bilateral. Acrofacial and Generalized vitiligo This is the most common type of viitligo. It typically begins on the fingers and the feet, around the mouth and eyes. At this stage it is called acrofacial vitiligo. Most commonly it then spreads to involve the arms, neck, chest, genitalia and legs. It doesn't often involve the back or if it does, it is confined to a small area over spine. Generalized vitiligo can manifest itself at any age and it is recorded as early as 3 or 4 years old as well as late in life, at 70 years old. After onset, the disease progresses slowly and intermittently for many years. Other common areas it affects are: the face, neck, dorsal and ventral forearms, axillae, inner thighs and knees. SOURCES: Vitiligo Vulgaris James J. Nordlund, I. Caroline Le Poole, and Raymond E. Boissy
In order for repigmentation to occur in vitiligo, pigment cells must be found in one of these three locations: the hair follicle unit, the border of a vitiligo lesion or unaffected melanocites within depigmented areas. Pigment cells found in the bulge region of the hair follicle are the most important sources for providing immature pigment cells that originate repigmentation. Melanocytes are present in large numbers in hair follicles and when stimulated they migrate towards the skin. An interesting fact is that regions lacking hair such as palms, soles and mucosal areas are particularly resilient to therapy because the melanocyte reservoir is missing . However a diffuse repigmentation pattern is seen, raising the question of an additional reservoir in the rete pegs outside the hair follicle. In order for repigmentation to occur from hair follicles it is necessary to stimulate melanocyte production (using UV treatment) and migration toward affected skin. Ultraviolet light is know to produce two effects on vitiligo skin: immunosuppresion (stop melanocite destruction) and stimulation of growth factors.
A bill initiated in by Brazilian representative José Olimpio pursues hospitals to provide psychological assistance to people with vitiligo. The text proposes that psychological treatment could be offered after an initial assessment by a psychologist. The representative pointed out that vitiligo patients can be more successful in their treatment after counseling: "Often, people go into depression when diagnosed with the disease. This further aggravates the situation", he writes. The project is to be further analyzed by a committee before being brought forward. Project text and status: https://www.camara.leg.br/proposicoesWeb/fichadetramitacao?idProposicao=496438 update: it appears the bill has been adopted in 2015. Can anyone with Brazilian Portuguese language skills leave a comment about what this actually means for vitiligo patients in Brazil?
The Koebner phenomenon refers to the development of new lesions following skin trauma. This occurs in patients with certain skin disease in areas of traumatized but otherwise normal skin. The new lesions are clinically identical to those in diseased skin. Koebner is not common only to vitiligo. It has been observed in other common skin conditions such as psoriazis, eczema and other rarer diseases. In fact, Heinrich Koebner, the dermatologist who first described it, made his initial observations on patients with psoriasis appearing at the site of horse bites or tattoos.
Some dermatologists recommend patients to cosmetically cover their vitiligo spots. This is associated with an improved quality of life since it reduces public stares or remarks. On the downside, covering up with makeup is time consuming - interfering with daily activities and in some cases, distress generating – the concern of permanently hiding something These opaque foundations are especially designed to mask skin disorders such as vitiligo and are different from normal makeup. On the downside, male patients aren’t comfortable wearing makeup and might get annoyed by a product rubbing against the shirt collar or cuffs. Other issues include the difficulty to match someone’s exact skin tone or the fact the color might wash on water contact. Microskin This article will review 5 products used as cosmetic camouflages for vitiligo Microskin
Following a strict plan of UV sessions like the one needed for vitiligo treatment can be a daunting task. Up to 6 months of home photo-therapy with 3 or 4 weekly sessions take a lot of time. Missing out on a UV session can result in a decrease of the overall efficiency of the treatment. This is where a smart-phone can come in handy. I've set 3 weekly reminders in the calendar of my Nokia phone in order to receive a screen notification each day a photo-therapy session is due. The reminder triggers an audio alarm in the evening, around the treatment time. To keep track of the exposure times for different spots, I use a mobile application. It's known that in vitiligo, body parts react differently to UV radiation. For example the hands require more treatment time then the face to achieve the slight reddening. This is why precise timing is a key factor during a treatment plan. The application can be used as a countdown timer during the actual photo-therapy session: an audio alarm is played when the exposure time is exhausted, notifying you to proceed to the next body part. The timers can be suggestively named with the exposed body part eg: face, neck, left hand, foot as in the screen-shots below. Each timer is editable allowing gradual increase of the exposure time.